Ankle Sprains
Inversion vs Eversion Injuries Explained
Ankle sprains are one of the most common musculoskeletal injuries across all age groups, affecting athletes, active individuals, and the general population alike. While often dismissed as “just a sprain,” ankle sprains can lead to long-term instability, recurrent injury, and chronic pain if not properly assessed and managed.
Understanding the type of ankle sprain is essential for appropriate treatment and recovery.
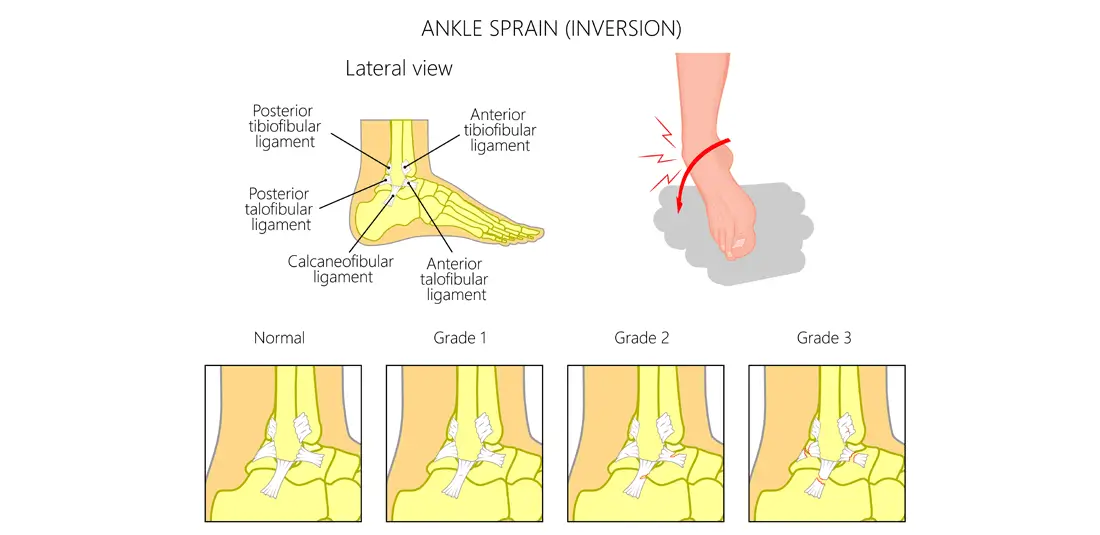
What Is an Ankle Sprain?
An ankle sprain occurs when the ligaments supporting the ankle joint are stretched or torn either partially or completely due to excessive force. Ligaments are strong bands of connective tissue that stabilise joints by limiting excessive movement.
Sprains typically happen when the ankle is forced beyond its normal range of motion during activities such as walking on uneven ground, sports, or sudden directional changes.
Inversion vs Eversion Sprains: What’s the Difference?
Inversion Ankle Sprain (Most Common)
An inversion sprain occurs when the foot rolls inwards, placing excessive stress on the ligaments on the outside (lateral side) of the ankle.
This commonly affects:
- Anterior talofibular ligament (ATFL)
- Calcaneofibular ligament (CFL)
It is also possible to sprain the posterior talofibular ligament (PTFL), however this injury is less typical.
Why it’s common:
The lateral ankle ligaments are structurally weaker and more vulnerable, especially during landing, cutting, or sudden changes in direction.
Typical symptoms include:
- Pain on the outer ankle
- Swelling and bruising
- Difficulty standing and walking
- A feeling of ankle instability
Eversion Ankle Sprain (Less Common, Often More Severe)
An eversion sprain occurs when the foot rolls outwards, stressing the ligaments on the inside (medial side) of the ankle. This primarily involves the deltoid ligament, a strong and complex structure.
Because the deltoid ligament is very robust, eversion injuries often involve higher forces and may be associated with:
- Bone bruising
- Fractures
- Syndesmotic (high ankle) injuries
Typical symptoms include:
- Pain on the inner ankle
- Significant swelling
- Difficulty walking
- Tenderness along the medial ankle
How Do Ankle Sprains Happen?
Common mechanisms include:
- Stepping on uneven surfaces
- Sudden changes in direction
- Poor landing mechanics
- Inadequate or incorrect footwear
- Previous ankle injury (a major risk factor)
Individuals with reduced balance, weakened ankle muscles, or poor proprioception (joint position awareness) are more susceptible to recurrent sprains.
How Are Ankle Sprains Diagnosed?
Diagnosis begins with a comprehensive clinical assessment, not just imaging.
Assessment typically includes:
- Injury mechanism history
- Swelling, bruising, and pain location
- Ligament stability testing
- Weight-bearing tolerance
- Foot and lower-limb biomechanics
- Gait assessment
Imaging such as X-ray, ultrasound, or MRI may be required if:
- Fracture is suspected
- Pain is severe or persistent
- Recovery is not progressing as expected
Why Proper Treatment Matters
An improperly managed ankle sprain can lead to:
- Chronic ankle instability
- Recurrent sprains
- Ongoing swelling and pain
- Reduced confidence in movement
- Increased risk of falls or secondary injuries
Simply “resting until it feels better” is often not enough.
Evidence-Based Treatment Approach
Acute Phase Management
Initial treatment focuses on:
- Reducing pain and swelling
- Protecting the injured ligaments
- Maintaining safe movement where possible
This may involve activity modification, bracing, or short-term support rather than complete immobilisation. In cases where pain, swelling, or tissue sensitivity persists, adjunctive therapies may be used to support healing alongside rehabilitation.
Extracorporeal Magnetotransduction Therapy (EMTT) is a non-invasive treatment that uses high-energy magnetic pulses to stimulate tissue repair. The magnetic field can penetrate deeper tissues, supporting blood flow, cellular activity, and pain modulation.
EMTT may be considered for:
- Persistent or slow-healing ankle sprains
- Ongoing ligament or tendon sensitivity
- Recurrent ankle injuries
It is used in conjunction with, not instead of, rehabilitation, strengthening, and biomechanical management. Suitability is determined on an individual basis following clinical assessment.
Rehabilitation and Strengthening
Rehabilitation is critical and often overlooked. This includes:
- Progressive strengthening of ankle and lower-limb muscles
- Balance and proprioception training
- Controlled return to impact and directional movements
These steps help restore stability and reduce re-injury risk.
Footwear and Orthotic Support
Footwear advice and, where appropriate, orthotic therapy can:
- Improve ankle alignment
- Reduce excessive strain
- Enhance shock absorption
- Improve confidence during walking or sport
Return-to-Activity Planning
A guided return to work, sport, or daily activity is essential. Returning too quickly significantly increases re-injury risk.
When Should You See a Podiatrist?
You should seek assessment if:
- Pain or swelling persists beyond a few days
- You cannot bear weight comfortably
- The ankle feels unstable or “gives way”
- You’ve had multiple ankle sprains
- You want a structured, safe return to activity
Early assessment reduces recovery time and prevents chronic issues.
Our Approach
At our clinic, ankle sprains are treated with a thorough biomechanical assessment and structured rehabilitation plan, tailored to the individual’s activity level and goals. We focus on restoring stability, confidence, and long-term ankle health rather than short-term symptom relief.
If you’ve recently injured your ankle or have ongoing issues from a past sprain, professional assessment can make a significant difference.
