Plantar Fasciitis
Causes, Symptoms, and Evidence-Based Treatment
Plantar fasciitis is one of the most common causes of heel pain seen in clinical practice. Despite its prevalence, it is frequently misunderstood, misdiagnosed, or oversimplified. At our clinic, we focus on identifying why plantar fasciitis has developed and addressing the underlying mechanical and load-related factors driving the condition.
What Is Plantar Fasciitis?
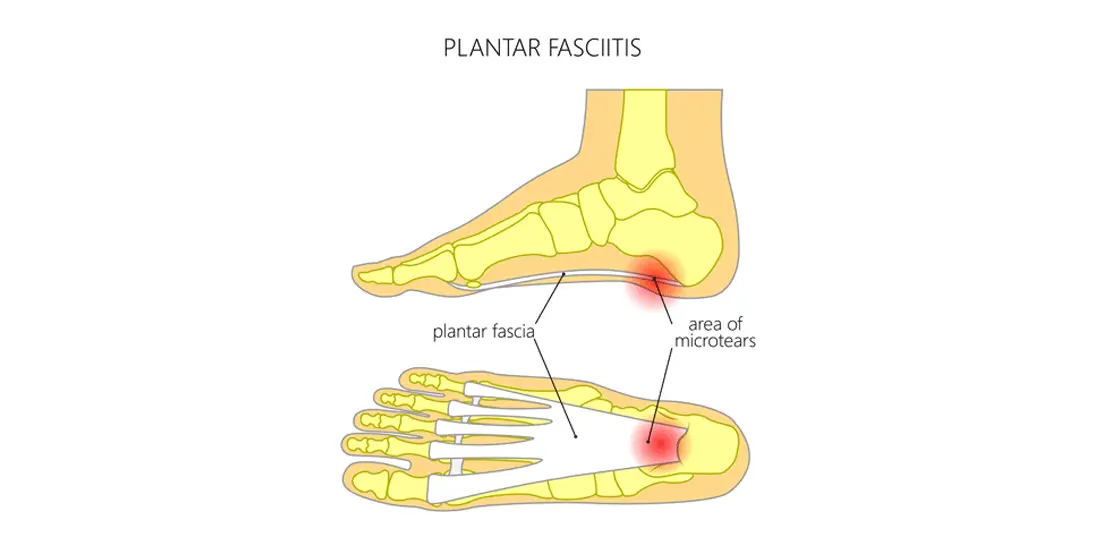
The plantar fascia is a thick, fibrous band of connective tissue that runs from the heel bone (calcaneus) to the toes. Its primary role is to support the arch of the foot and assist with efficient load transfer during walking, running, and standing.
Plantar fasciitis refers to pain originating from this structure, most commonly at its starting point at the heel. While the name suggests inflammation, current evidence shows that many cases involve degenerative changes in the tissue rather than acute inflammation. In simple terms, the fascia becomes overloaded, strained, and unable to recover adequately between activities.
Common Symptoms
Plantar fasciitis typically presents with:
- Heel pain that is worst with the first step in the morning
- Pain after prolonged sitting or rest
- Discomfort that improves slightly with movement but worsens after long periods on your feet
- Localised tenderness at the inside of the heel
- Tightness in the calf or arch
Pain may be mild and intermittent initially, but without appropriate management, it can become persistent and limiting.
Why Does Plantar Fasciitis Develop?
Plantar fasciitis is rarely caused by a single factor. Instead, it develops due to cumulative overload of the plantar fascia. Common contributing factors include:
Biomechanical Factors
These relate to how your foot and lower limb move and load:
- Reduced ankle dorsiflexion (limited upward movement of the ankle)
- Excessive pronation or supination during gait
- Poor shock absorption
- Reduced intrinsic foot muscle strength
Load and Activity Changes
Sudden changes in activity often precede symptoms:
- Increase in running or walking volume
- Change in training surface
- Return to activity after a period of inactivity
- Occupations requiring prolonged standing
Footwear Factors
Shoes that lack adequate support or cushioning can increase strain on the plantar fascia, particularly:
- Minimal or worn-out footwear
- Unsupportive work shoes
- Inappropriate running shoes for your biomechanics
How Is Plantar Fasciitis Diagnosed?
Diagnosis is primarily clinical, based on a detailed history and physical examination. Imaging such as ultrasound can be used to confirm diagnosis.
A thorough assessment will look at:
- Foot posture and arch behaviour
- Ankle and calf flexibility
- Gait mechanics
- Load tolerance and activity history
- Footwear habits
This approach allows treatment to be tailored rather than generic.
Treatment: What Actually Works?
There is no single “quick fix” for plantar fasciitis. Effective management focuses on load modification, tissue capacity, and mechanical support.
Load Management
Reducing aggravating activities temporarily while maintaining general fitness is crucial. This does not mean complete rest, but rather controlled, strategic loading.
Stretching and Strengthening
Targeted exercises may include:
- Calf stretching to reduce strain on the fascia
- Plantar fascia–specific stretching
- Progressive strengthening of foot and lower-limb muscles
Footwear Advice
Appropriate footwear can significantly reduce symptoms by improving load distribution and shock absorption.
Orthotic Therapy
Custom orthotics may be prescribed to:
- Support the arch
- Reduce excessive strain on the plantar fascia
- Improve overall foot mechanics
These are prescribed based on assessment findings, not as a one-size-fits-all solution.
Adjunctive Therapies
Depending on presentation, additional treatments may include:
- Shockwave therapy
- Extracorporeal magnetotransduction therapy
- Taping techniques
- Manual therapy to address joint or soft-tissue restrictions
When Should You See a Podiatrist?
You should seek professional assessment if:
- Heel pain persists beyond two to three weeks
- Pain is worsening or limiting daily activity
- You experience pain on both feet
- Self-management has not helped
Early intervention leads to faster recovery and reduces the risk of chronic symptoms.
Our Approach
At our clinic, plantar fasciitis is managed through detailed biomechanical assessment, clear explanation, and evidence-based treatment planning. We prioritise long-term resolution rather than short-term symptom suppression, ensuring patients understand their condition and play an active role in recovery. We work with each individual to create a treatment plan that suits their needs as well as their lifestyle.
If you’re experiencing heel pain or suspect plantar fasciitis, a proper assessment can make all the difference
